AARP Hearing Center
Key details
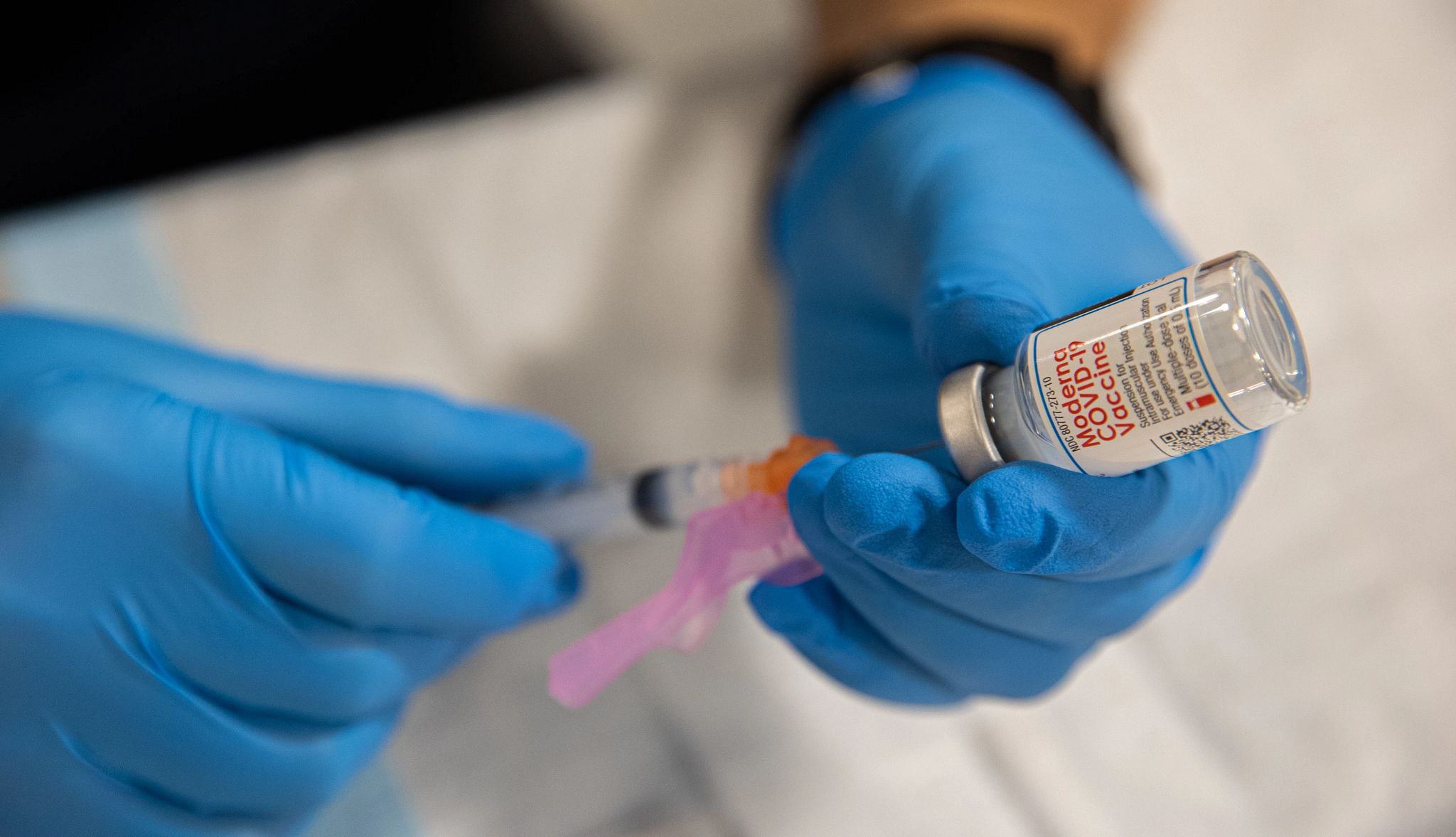
- Updated versions of the Pfizer and Moderna vaccines have been approved for the 2024-2025 season and they target a more recent strain of the virus called KP.2 that was behind much of this summer’s surge in COVID-19 cases.
- An updated version of the Novavax vaccine has been approved for the 2024-2025 season. It will target JN.1, which is the parent strain of KP.2 and other circulating variants.
- It’s recommended that nearly everyone get an updated vaccine once it is available.
- Vaccines are available at pharmacies, clinics and doctor’s offices. Search for vaccination sites by ZIP code at Vaccines.gov.
Which vaccines are available, and who can get them?
The Centers for Disease Control and Prevention (CDC) says everyone 6 months and older should get an updated 2024-2025 COVID-19 vaccine.
Pfizer and Moderna: The updated mRNA vaccines were approved by the U.S. Food and Drug Administration (FDA) in August and replace previous versions of the vaccine. The CDC recommends that people 6 months and older get the updated vaccine (no longer referred to as a booster), which targets a more recent strain of the omicron variant.
People 5 and older — and especially adults age 65 and older, those living in a long-term care facility, and those who are at high risk of severe disease from a coronavirus infection — should get one dose of the updated vaccine, regardless of how many and which vaccines they previously received. Children 6 months to 4 years old may need more than one shot, depending on their age and vaccination status, according to CDC recommendations.
Novavax: The vaccine uses a more traditional (protein-based) technology and has been authorized by the FDA for people 12 and older. Novavax’s vaccine for 2024-2025 replaces previous versions of the vaccine. It targets the parent strain of circulating variants.
You will need two shots given three weeks apart for a full primary series. You may get a single dose if you’ve been previously vaccinated at least two months before and have not received an updated Pfizer or Moderna mRNA vaccine.
People with compromised immune systems may receive additional doses, depending on their vaccination history. More information is available at the CDC’s website.
Where can I get a vaccine?
Use the federal government’s website Vaccines.gov to search for vaccination sites by ZIP code. Get the same information by texting your ZIP code to 438829 or by calling 800-232-0233. Vaccines are administered at retail pharmacies, including Walgreens, Walmart and CVS; clinics; and other locations, such as doctor’s offices. Check with your primary care physician’s office to see if COVID-19 vaccinations are offered. If you are a veteran, the Department of Veterans Affairs offers COVID-19 vaccinations at VA facilities. Sign up online or call 800-827-1000 to make an appointment.
Visit Massachusetts’ Department of Public Health COVID-19 vaccine information webpage or call its 211 hotline for information about state-sponsored vaccination sites, such as local health departments, community health centers and mobile vaccination clinics.
Do I have to pay for the vaccination?
The federal government no longer covers the cost of the vaccines, but most people with Medicare, Medicaid or private insurance will not have to pay out of pocket for the shot.
If you are uninsured, contact your local or state public health department or a nearby federally qualified health center about vaccination opportunities.
Children 18 and younger may qualify to receive no-cost or low-cost vaccines through the federal Vaccines for Children (VFC) Program.
What should I bring to my vaccine appointment?
Some vaccination sites ask for proof of identity or eligibility. Bring a driver’s license or other state-issued ID that shows your name, age and state residency, along with your health insurance card.
Do I need to bring my vaccine card?
The CDC no longer distributes COVID-19 vaccine cards, and they are not required to receive a vaccine. If you would like one, however, you can request a digital COVID-19 vaccine card — called a COVID-19 SMART Health Card in Massachusetts — at the state’s MyVaxRecords website. If a record of your vaccination is unavailable on MyVaxRecords, contact the provider who administered your vaccine to have them update your MyVaxRecords or provide you with the record directly.
What are the side effects of the COVID-19 vaccine?
It’s not uncommon to experience mild to moderate side effects after getting vaccinated, such as soreness in the arm, headache, fatigue, muscle and joint pain, nausea, fever or chills — but these are temporary “and normal signs that your body is building protection,” the CDC says.
A small number of vaccine recipients have experienced adverse reactions to the shots.
Can I get the COVID-19, RSV and flu vaccines at the same time?
According to the CDC, it is safe to receive the flu vaccine and updated COVID-19 vaccines simultaneously, although you are a little more likely to experience side effects, such as a headache and fatigue. Adults 75 or older (and those 60 to 74 with certain underlying health conditions) who are encouraged to get the RSV vaccine may receive that at the same time as the others, but some health experts suggest spacing them out. If you had the RSV vaccine last year, you don’t need another one this year.
Contact your health care provider for more information.
How are vaccinations working in nursing homes and long-term care facilities?
The U.S. government no longer distributes COVID-19 vaccines to long-term care facilities. That means nursing homes, assisted living facilities and other long-term care settings are responsible for coordinating COVID-19 vaccination programs for their residents and staff. Most long-term care facilities have partnerships with pharmacies or health departments to provide vaccines for flu, COVID-19 and other illnesses.
Long-term care facilities that receive Medicare and/or Medicaid dollars are required by federal law to educate residents, their representatives and staff about COVID-19 vaccines and offer a COVID-19 vaccine to residents, resident representatives and staff.
How protected am I postvaccination?
All vaccines reduce the risk of COVID-19 infections and are highly effective at preventing severe illness and death from the disease. No vaccine is 100 percent effective, and infections can still occur postvaccination.
How can I avoid COVID-19 scams?
Be aware that scammers often purport to offer COVID-19 vaccines and treatments and try to charge for them. The AARP Fraud Watch Network is tracking the latest scams.
Massachusetts residents who believe they’ve encountered a COVID-19 scam can report it to the U.S. Department of Health and Human Services Office of Inspector General by calling 800-447-8477 or by submitting a complaint online.
Editor's note: This guide was first published Jan. 13, 2021, and has been updated with new information.
Emily Paulin is a reporter for AARP covering nursing homes, health care, and federal and state policy. Her work has also appeared in Broadsheet, an Australian lifestyle publication.
Also of Interest:
7 Things to Know About the New COVID-19 Vaccines
What to Know About New COVID-19 Variants
What Older Adults Should Know About COVID-19































































