AARP Hearing Center
By Vince McKelvey
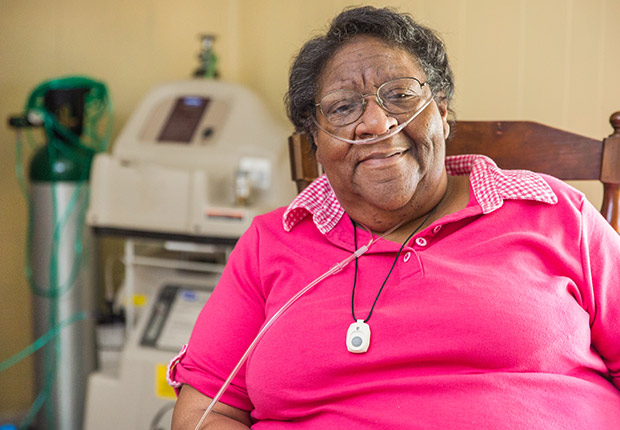
Donna Flucas, of suburban Dayton, was not yet 50 when health issues forced her to leave her job in procurement at Wright-Patterson Air Force Base.
As her pulmonary disease progressed, her medications became unaffordable, even with health insurance, said Flucas, 68, who also has other ailments.
About a year ago she learned that she qualified for PASSPORT, an Ohio Medicaid program created in 1986 that helps many of those 60 and older stay in their homes. Now her prescriptions are covered through Medicaid, Medicare and her insurance. In addition, Medicaid pays her Medicare premiums and for regular visits from a home health aide.
“I can’t tell you how much it’s helped me,” she said.
Medicaid, the federal-state health insurance program, has been helping low-income people for 50 years. The federal law establishing both Medicaid and Medicare was signed on July 30, 1965. Before that, medical care for the poor was seen as inadequate.
“We had a lot of people who were economically fragile, who just didn’t have access to any services,” said Sarah Twill, chair of the social work department at Wright State University in Dayton.
In the past half century, Medicaid has evolved from a program that primarily covered pregnant women, children and people in nursing homes to one that also covers the working poor and home care.
In recent years, a major aspect of that shift has been to provide long-term care services that help people remain in their homes rather than in an institution. In 2014, for the first time, the state spent more on home- and community-based services than on institutional care.
Luke Russell, AARP Ohio advocacy director, acknowledged the need for nursing homes. But he said people strongly prefer to stay at home, which contributes to their well-being, and that home care costs much less than institutional care.
State expanded coverage
Nearly 3 million people in Ohio are covered by Medicaid, including 492,000 who qualified when Gov. John Kasich (R) expanded the program in 2014 under the federal Affordable Care Act (ACA) to cover individuals with incomes up to about $16,200. AARP Ohio strongly supported the expansion. About 17 percent of the new beneficiaries are 55 to 64.
The federal and state governments share the cost of Medicaid. The federal government currently pays the full cost of those covered by the expansion—which will gradually diminish to 90 percent by 2020. For those covered under the pre-expansion rules, the federal government provides $1.68 for each $1 the state spends.
As part of the ACA, Ohio received an additional $169 million in federal funds to enhance services that help older people and those with disabilities remain in their homes and communities.
Roughly 80 percent of Ohioans covered by Medicaid are insured through private managed care plans. Managed care supplanted a fee-for-service approach in which people could choose a health care provider and the state paid the bill. Now the state makes a monthly payment to health insurers.
Sam Rossi, Ohio Medicaid communications director, said managed care helps control costs and offers better coordination of patients’ medical care. “We monitor them,” he said. “There are performance measures that we look at.... We want high quality from our plans.”
Rossi said the Kasich administration sets a priority on supporting home care. For example, since 2011, the state’s HOME Choice program has helped over 5,000 people move from nursing homes into community settings. What’s more, waiting lists have been eliminated from the state’s PASSPORT program.
Flucas is happy at home. She has strong family support, including grandchildren who live in the area, and where she hosts family dinners one Sunday a month. “Right now I try to stay as independent as I can, and it’s working out for me.”
To find in-home care providers, contact the Ohio Department of Aging at 866-243-5678 toll-free.
Vince McKelvey is a freelance writer based in Dayton, Ohio.































































